A recent Research Letter published in The Journal of the American Medical Association or JAMA provides us with insight regarding the functioning of the American medical system, particularly, the relationship between physicians and Big Pharma. In the article, the authors examined data from the federal government's Open Payment platform which records payments to physicians from the health care industry, focusing on physicians in specialty practices. Open Payments was established under the Physician Payments Sunshine Act in August 2013 in an effort to ensure that patients would have the ability to discern whether financial conflicts of interest may influence physicans' prescribing histories. Data for physicians are available in a searchable database by either physician name or hospital and, over the past two years includes payments to physician assistants, nurse practitioners, clinical nurse specialists, certified registered nurse anesthetists, anesthesiologist assistants and certified nurse midwives. Payments include but are not limited to research, meals, speaking fees, travel, entertainment, education, grants, charitable donations, honoraria and gifts noting that there is an absence of data on certain types of payments like free drug samples..
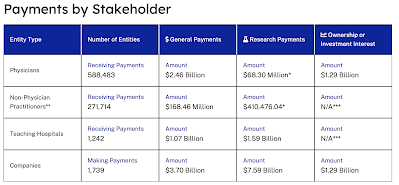
For 2022 alone (the latest year for which data is available), industry made 14.11 million payments totalling $12.58 billion US to physicians as shown here:
Going back to the study as a whole, the authors found that between 2013 and 2022, 85,087,744 payments were made by industry to 826,313 of 1,445,944 eligible physicians across 39 specialties with the median payment of $48 per physician. The highest annual total value was $1.60 billion in 2019 and the lowest was $863.93 million in 2020. Let's look at some details:
1.) Highest sum of payments by specialty:
- orthopaedic surgeons - $1.36 billion (31,620 recipients)
- neurologists/psychiatrists - $1.32 billion (58,688 recipients)
- cardiologists - $1.29 billion (33,074 recipients)
- hematologists/oncologists - $825.8 million (17,025 recipients)
- general internal medicine - $588.2 million (97,542 recipients)
Payments were highly skewed with the payments to median physicians ranging from $0 to $2339 compared to $194,933 for the top 0.1 percent of hospitalists and $4,826,944 for the top 0.1 percent of orthopaedic surgeons.
2.) Highest sum of payments by drug:
- Zarelto - $176.34 million
- Elequis - $102.62 million
- Humira - $100.17 million
Other drugs associated with high payments include Invokana, Jardiance, Farxiga, Dupixent, Botox and Keytruda.
3.) Highest sum of payments by medical device:
- da Vinci Surgical System - $307.52 million
- Mako SmartRobotics - $50.13 million
- CoreValve Evolut - $44.79 million
Other devices with high payments include Natrelle Implants, Impella, Sapien 3 and Arthrex Devices.
During the pandemic, it became quite obvious that many physicians had very close relationships with the medical industry, in particular, the pharmaceutical arm of the business. It is quite apparent that the health care industry directs payments of various types to physicians to influence their practices and preferences; by directing payments to physicians and other medical professionals, the health care industry is anticipating greater profits. After all, they aren't making billions of dollars of payments to their customers without expecting a significant return on their "investments". Unfortunately, these investments have the potential to create conflicts of interest with some physicians potentially making life and death decisions for their patients based on the influence of their benefactors.